Healthy, Wealthy And Wise-- Ro Khanna & Mark Pocan Have An Idea
- Howie Klein

- Oct 16, 2022
- 6 min read

Yesterday I got a letter from the Medicare administration folks and you can see part of it above. I’m a huge Medicare supporter and I feel like it saved my life. When I was diagnosed with a rare former of cancer— mantle cell lymphoma— treatment was well over a million dollars. Who can afford that! Medicare paid everything without any of the tricks private insurance companies use to not pay.
On Friday, I was very happy to see a new bill by Ro Khanna and Mark Pocan, the Save Medicare Act, meant to prevent for-profit (and nothing else) insurance companies from tricking people into thinking they are part of Medicare. Khanna, explaining the bill to his constituents, wrote that ahead of Medicare's Open Enrollment period, he and Pocan are seeking to “prohibit private insurers from using ‘Medicare’ in plan titles or advertisements, and impose significant fines for any insurer that engages in this deceptive practice.”
He explained that “‘Medicare Advantage’ is just private insurance that profits by denying coverage and the name is being used to trick seniors into enrolling. That’s not right. This bill will prevent these private insurers from labeling themselves as ‘Medicare’ and allow us to focus on strengthening and expanding real Medicare instead.”
Pocan said that “Only Medicare is Medicare. It is one of the most popular and important services the government provides. We should be working to expand this service to include coverage for dental, vision, and hearing care, as well as looking at ways to strengthen it rather than allowing these ‘Medicare Advantage’ programs to provide pale alternatives to what Medicare does. These non-Medicare plans run by private insurers undermine traditional Medicare. They often leave patients without the benefits they need while overcharging the federal government for corporate profit. This bill eliminates any confusion about what is– and what is not– Medicare, and ensures this essential program will continue to serve seniors and other Americans for years to come.”
Former insurance executive Wendell Potter, President of the Center for Health and Democracy, weighed in in favor of the bill: “So-called Medicare Advantage is neither Medicare nor an advantage. It is simply another scheme by the insurance companies to line their pockets at the expense of consumers. I applaud Congressman Pocan and Congressman Khanna for introducing this vital legislation. The health care market is confusing for consumers and misleading branding like so-called Medicare Advantage just makes it worse.”
According to a recent New York Times article, “8 of the 10 largest Medicare Advantage insurers– representing more than two-thirds of the market– have submitted inflated bills…and four of the five largest players– United Health, Humana, Elevance, and Kaiser– have faced federal lawsuits alleging that efforts to overdiagnose their customers crossed the line into fraud.”
Additionally, according to the federal Medicare Payment Advisory Commission’s 2022 report to Congress, at least $12 billion in overpayments were made to Medicare Advantage plans in 2020 by the federal government.
The “Save Medicare Act” will eliminate the confusion private insurers have relied upon for years to enroll unsuspecting seniors, and restore true Medicare as the primary health plan older Americans rely on.
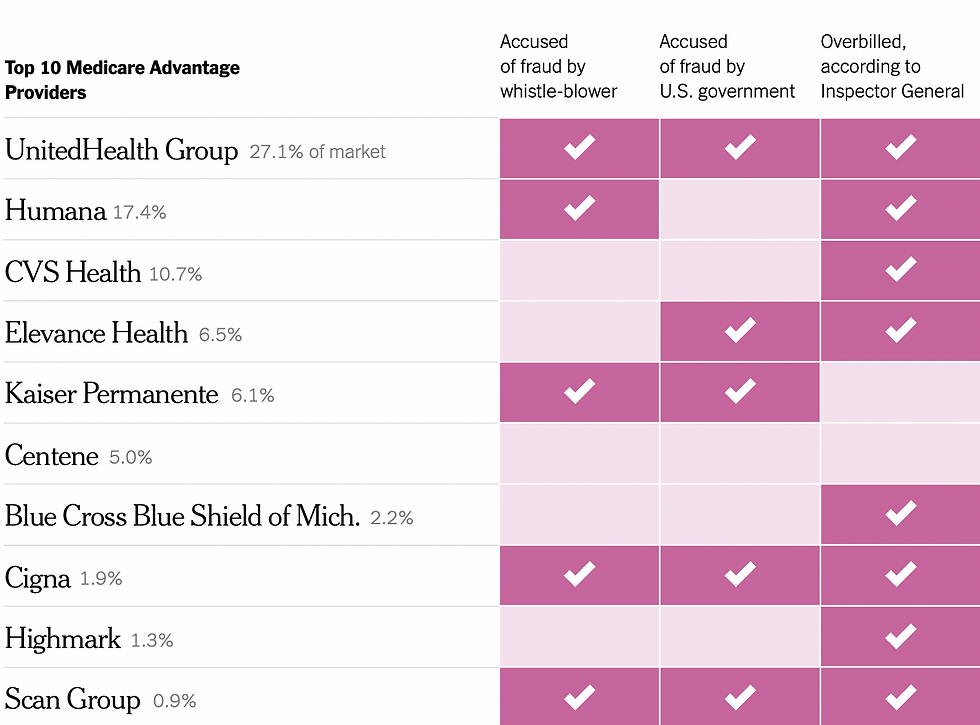
The NY Times piece they referenced noted that “Kaiser Permanente called doctors in during lunch and after work and urged them to add additional illnesses to the medical records of patients they hadn’t seen in weeks. Doctors who found enough new diagnoses could earn bottles of Champagne, or a bonus in their paycheck.” Similarly, Anthem (a crooked insurance company that changed its name to Elevance Health) “paid more to doctors who said their patients were sicker. And executives at UnitedHealth Group, the country’s largest insurer, told their workers to mine old medical records for more illnesses— and when they couldn’t find enough, sent them back to try again.” Sounds like the executives who run these places could successfully run for governor and senator of Florida.
Reed Abelson and Margot Sanger-Katz, the two Times reporters wrote that the 2 strategies, “which were described by the Justice Department in lawsuits against the companies— led to diagnoses of serious diseases that might have never existed. But the diagnoses had a lucrative side effect: They let the insurers collect more money from the federal government’s Medicare Advantage program.” Their “review of dozens of fraud lawsuits, inspector general audits and investigations by watchdogs shows how major health insurers exploited the program to inflate their profits by billions of dollars.”
The government pays Medicare Advantage insurers a set amount for each person who enrolls, with higher rates for sicker patients. And the insurers, among the largest and most prosperous American companies, have developed elaborate systems to make their patients appear as sick as possible, often without providing additional treatment, according to the lawsuits.
As a result, a program devised to help lower health care spending has instead become substantially more costly than the traditional government program it was meant to improve.
Eight of the 10 biggest Medicare Advantage insurers— representing more than two-thirds of the market— have submitted inflated bills, according to the federal audits. And four of the five largest players— UnitedHealth, Humana, Elevance and Kaiser— have faced federal lawsuits alleging that efforts to overdiagnose their customers crossed the line into fraud.
The fifth company, CVS Health, which owns Aetna, told investors its practices were being investigated by the Department of Justice.
… The increased privatization has come as Medicare’s finances have been strained by the aging of baby boomers. But for insurers that already dominate health care for workers, the program is strikingly lucrative: A study from the Kaiser Family Foundation, a research group unaffiliated with the insurer Kaiser, found the companies typically earn twice as much gross profit from their Medicare Advantage plans as from other types of insurance.
For people choosing between traditional Medicare and Medicare Advantage, there are trade-offs. Medicare Advantage plans can limit patients’ choice of doctors, and sometimes require jumping through more hoops before getting certain types of expensive care.
But they often have lower premiums or perks like dental benefits— extras that draw beneficiaries to the programs. The more the plans are overpaid by Medicare, the more generous to customers they can afford to be.
…The popularity of Medicare Advantage plans has helped them avoid legislative reforms. The plans have become popular in urban areas, and have been increasingly embraced by Democrats as well as Republicans. Nearly 80 percent of U.S. House members signed a letter this year saying they were “ready to protect the program from policies that would undermine” its stability.
“You have a powerful insurance lobby, and their lobbyists have built strong support for this in Congress,” said Representative Lloyd Doggett, a Texas Democrat who chairs the House Ways and Means Health subcommittee.
Some critics say the lack of oversight has encouraged the industry to compete over who can most effectively game the system rather than who can provide the best care.
…Congress’ first attempt to design a privatized Medicare plan paid insurers the same amount for every patient with similar demographic characteristics.
In theory, if the insurers could do better than traditional Medicare— by better managing patients’ care, or otherwise improving their health— their patients would cost less and the insurers would make more money.
But some insurers engaged in strategies— like locating their enrollment offices upstairs, or offering gym memberships — to entice only the healthiest seniors, who would require less care, to join. To deter such tactics, Congress decided to pay more for sicker patients.
Almost immediately, companies saw ways to exploit that system. The traditional Medicare program provided no financial incentive to doctors to document every diagnosis, so many records were incomplete. Under the new program, insurers began rigorously documenting all of a patient’s health conditions— say depression, or a long-ago stroke— even when they had nothing to do with the patient’s current medical care.
…Kaiser, which both runs a health plan and provides medical care, is often seen as a model system. But its control over providers gave it additional leverage to demand additional diagnoses from the doctors themselves, according to the lawsuit.
“The cash monster was insatiable,” said Dr. James Taylor, a former coding expert at Kaiser who is one of 10 whistle-blowers to accuse the organization of fraud.
At meetings with supervisors, he was instructed to find additional conditions worth tens of millions of dollars. “It was an actual agenda item and how could we get this,” Dr. Taylor said.
…The Justice Department has brought or joined 12 of the 21 cases that have been made public. But whistle-blower cases remain secret until the department has evaluated them. “We’re aware of other cases that are under seal,” said Mary Inman, a partner at the firm Constantine Cannon, which represents many of the whistle-blowers.
But few analysts expect major legislative or regulatory changes to the program.
“Medicare Advantage overpayments are a political third rail,” said Dr. Richard Gilfillan, a former hospital and insurance executive and a former top regulator at Medicare, in an email. “The big health care plans know it’s wrong, and they know how to fix it, but they’re making too much money to stop. Their C.E.O.s should come to the table with Medicare as they did for the Affordable Care Act, end the coding frenzy, and let providers focus on better care, not more dollars for plans.”
It will be more than a little interesting to see which members of Congress have the guts to co-sponsor Khanna’s and Pocan’s Save Medicare Act. It’s going to be very tough for the members of Congress who run their careers based on legalistic bribery and corruption.We’ll be watching, of course.




any idea why it took them 2 years to do this?